(503) 966-3780
The Ultimate Guide to Dental Predeterminations
By Progressive Periodontics
April 29, 2021
Dental insurance plans can be confusing and, in some cases, frustrating. Most plan booklets will show benefit levels ranging from 50% to 90%. Armed with those percentages, most patients pursue treatment expecting coverage. Imagine their surprise when they receive a bill from their treating dentist.
What most insurance plans don’t tell you is that those percentages are based on a fee schedule created by the insurance company. If you see a dentist of your choice who is not contracted with that insurance company, there is a good chance that percentages will be wrong. So, how does one go about getting a more accurate benefit estimate? The answer: A Dental Predetermination.
What is a dental predetermination?
A predetermination is an estimate from the dental insurance company that provides an estimated out of pocket portion for a proposed treatment plan. This form is different from a confirmation of coverage that is given over the phone by a customer service agent in that it provides an estimated dollar amount rather than an estimated percentage.
Why would you need a dental predetermination?
For treatment plans over $300, most dental insurance companies recommend that a dental predetermination be submitted. Most patients who opt for a predetermination do so to determine a better estimate of their financial liability before proceeding.
How long does a dental predetermination take?
While all carriers are different, most dental predeterminations take 4-6 weeks from the time that they are sent to the dental insurance company to the time that it is received back. The predetermination is sent with treatment records, radiographs, and other pertinent information to help the dental insurance company better determine medical necessity. This process can take longer if the insurance company requests additional information from the dental provider.
How to Read a Dental Predetermination
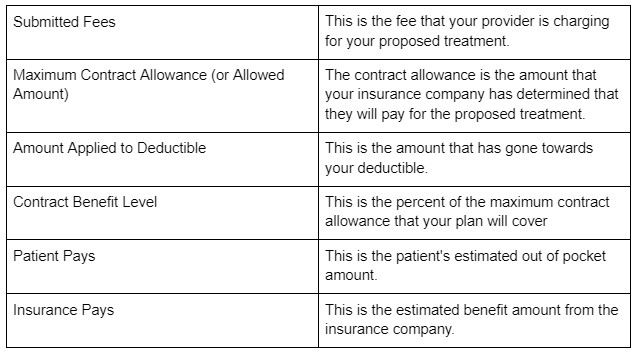
After the predetermination is processed by the insurance company, both the patient and the provider will receive a copy. From experience, the patient will often receive the predetermination a few days before the provider’s office. All dental insurance companies format their predeterminations a bit different. Some will clearly state that it is an estimate, while others will look very similar to an EOB (Explanation of Benefits) that is received after a claim has been processed. In any case, there will always be at least 6 columns.
When does a dental predetermination expire?
Most dental predeterminations expire 12 months after they’ve been issued. There are a few insurance companies (such as Delta Dental of Idaho) that state predeterminations expire 6 months after they are issued. A majority of the dental predeterminations will state their expiration date on the form.
Important things to note about dental predeterminations
While having a detailed estimate is helpful, it does not guarantee payment. In some situations, patients will complete other dental treatment before the predetermined treatment. This affects the remaining annual maximum, which then affects the payment made towards the predetermined treatment.
It’s important to know that some insurance companies may still deny your claim following treatment. Most provider’s offices can work with their patients to appeal the claim.
